- Search
| Ann Rehabil Med > Volume 42(1); 2018 > Article |
Abstract
Objective
Methods
Results
Conclusion
ACKNOWLEDGMENTS
CONFLICT OF INTEREST:
CONFLICT OF INTEREST: No potential conflict of interest relevant to this article was reported.
References
Fig. 1
Characteristics of included patients. (A) Site of primary cancer, (B) Eastern Cooperative Oncology Group (ECOG) performance scale, (C) Karnofsky performance scale, (D) Functional Ambulatory Category, and (E) level of ambulation. Others include ovary, esophagus, prostate, bone (osteosarcoma) and blood (leukemia).

Table 3
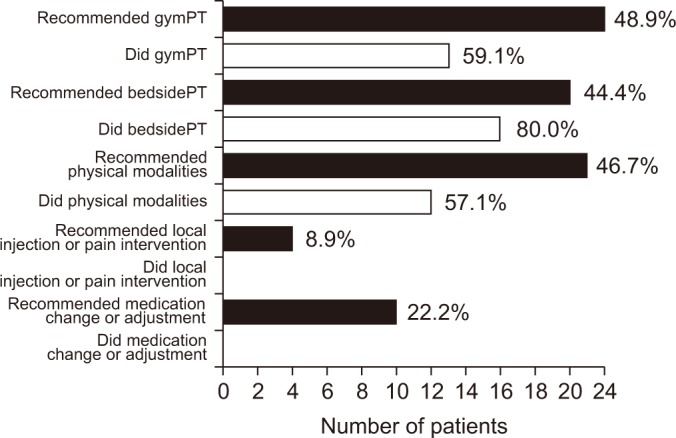
Compliance to rehabilitation approach

FAC, Functional Ambulatory Category; ECOG PS, Eastern Cooperative Oncology Group; PS, performance scale.
a)Patients followed rehabilitation recommendation for physical therapy at Gym.
b)Patients followed rehabilitation recommendation for physical therapy at bedside.
c)Patients followed rehabilitation recommendation for physical modalities.
*p<0.05.
Table 4
Result of satisfaction and dissatisfaction questionnaire

Values are presented as number (%) or mean±standard deviation (median).
a)Total patients were 13 who answered the survey by himself or by his/her care-giver.
b)Overall satisfaction score was surveyed with 11-point Likert scale (0–10).
c,d)Satisfaction and dissatisfaction score were calculated as sum of number which answered as positive within satisfaction/dissatisfaction items, each item scores 1 point.
Table 5
Correlations between patient characteristics and satisfaction

FAC, Functional Ambulatory Category; ECOG PS, Eastern Cooperative Oncology Group; PS, performance status.
a)Using 11-point Likert scale (0–10).
b)Get 1 point per each satisfaction item (0–5).
c)Get 1 point per each dissatisfaction item (0–5).
d)Satisfaction score minus dissatisfaction score.
*p<0.05.
- TOOLS
-
METRICS

- Related articles in ARM
-
Recent Trends in Rehabilitation for Cancer Patients2022 June;46(3)
Rehabilitation of Individuals With Cancer2022 April;46(2)
Cost of Rehabilitation Treatment of Patients With Cerebral Palsy in Korea2018 October;42(5)
Rehabilitation of Head Injury Patients, the Importance of Cognitive Therapy1996 March;20(1)
Rehabilitation of the Patients after Total Hip Replacement1992 June;16(2)