- Search
| Ann Rehabil Med > Volume 37(1); 2013 > Article |
Abstract
Objective
To examine the neurophysiologic status in patients with idiopathic facial nerve palsy (Bell's palsy) and Ramsay Hunt syndrome (herpes zoster oticus) within 7 days from onset of symptoms, by comparing the amplitude of compound muscle action potentials (CMAP) of facial muscles in electroneuronography (ENoG) and transcranial magnetic stimulation (TMS).
Methods
The facial nerve conduction study using ENoG and TMS was performed in 42 patients with Bell's palsy and 14 patients with Ramsay Hunt syndrome within 7 days from onset of symptoms. Denervation ratio was calculated as CMAP amplitude evoked by ENoG or TMS on the affected side as percentage of the amplitudes on the healthy side. The severity of the facial palsy was graded according to House-Brackmann facial grading scale (H-B FGS).
Results
In all subjects, the denervation ratio in TMS (71.53±18.38%) was significantly greater than the denervation ratio in ENoG (41.95±21.59%). The difference of denervation ratio between ENoG and TMS was significantly smaller in patients with Ramsay Hunt syndrome than in patients with Bell's palsy. The denervation ratio of ENoG or TMS did not correlated significantly with the H-B FGS.
The annual incidence of peripheral facial paralysis is 20 to 30 per 100,000 persons, among which Bell's palsy is the most common cause of the disease, constituting approximately 60% to 75% of the overall patients with acute facial nerve palsy [1]. The typical signs and symptoms of Bell's palsy include paresthesia of some parts of the ear and dysautonomia of the parotid gland, the gustatory sense in the anterior two-thirds of the tongue occurring through the chorda tympani nerve, and the lacrimal gland, as well as paralysis and attenuation of the muscles controlled by the facial nerve [2]. Ramsay Hunt syndrome, the keynote symptoms of which are facial nerve palsy, ear pain, and herpetic dermatomeric rash on the skull, is another common cause of facial paralysis. This disease is known to comprise about 12% of all patients with acute facial palsy [3]. Recent studies have reported that Bell's palsy and Ramsay Hunt syndrome result from herpes simplex virus type 1 (HSV-1) and varicella-zoster virus (VZV), respectively, each being reactivated after latent infection of the geniculate ganglion [4-7]. According to Fisch and Esslen's research [8], their examination of 3 patients with Bell's palsy revealed that nerve impulses were blocked at the proximal part of the geniculate ganglion and at the medial part of the internal acoustic canal when electrical stimulation was being performed on exposed facial nerve during middle cranial fossa decompression. Gantz et al. [9] also observed nerve conduction block at the proximal part of the geniculate ganglion on 69% of 16 patients suffering from Bell's palsy who showed denervation in 90% to 98% in the preoperative electroneuronography when in the same way electrical stimulation was performed on the facial nerve during operation. These studies together suggest that the initial lesions of Bell's palsy and of Ramsay Hunt syndrome may exist in upper part of the geniculate ganglion.
Early diagnosis is crucial to estimating a patient's prognosis for these 2 diseases because patients with Bell's palsy are expected to have a higher recovery rate than those with Ramsay Hunt syndrome, if the patient receives proper medical treatment [10]. Among a variety of electrical diagnosis/screening tests for such acute facial palsy, the facial nerve conduction test has been used for the prognosis of the disease. The recovery rate varies with the degree of denervation [11,12]. However, the validity of the electroneuronography falls short during the initial several days, before Wallerian degeneration of the facial nerve advances to the distal part of the stylomastoid foramen [13]. To overcome this drawback, studies have been carried out employing transcranial magnetic stimulation at the initial stage of the illness. The transcranial magnetic stimulation has the facial nerve of the internal acoustic canal depolarized through the magnetic field, giving rise to motor-evoked potential [14,15]. It has already been reported throughout previous literature that when transcranial magnetic stimulation was conducted on patients with Bell's palsy, the motor-evoked potential disappeared or decreased within several hours after the development of the symptoms [13,14]. Nowak et al. [16] confirmed that the motor-evoked potential decreased or disappeared in not only Bell's palsy, but also in Ramsay Hunt syndrome when transcranial magnetic stimulation was performed within 3 days after the development of the symptoms. Considering that the decrement of compound muscle action potential and the degree of facial palsy were more significant in Ramsay Hunt syndrome than in Bell's palsy, Nowak et al. [16] also suggested that more severe and faster axon damage may occur in facial palsy caused by VZV. However, there are few papers that have studied the differences between Bell's palsy and Ramsay Hunt syndrome comparing both the facial nerve conduction test and the transcranial magnetic stimulation test.
The present research has attempted to provide basic data for the diagnoses and prognoses of acute facial palsy patients after securing the neurophysiological differences between the 2 diseases, by comparing amplitude differences of compound muscle action potential in the facial nerve conduction test and the transcranial magnetic stimulation test on the healthy side (normal people) and on the affected side (patients with either Bell's palsy or Ramsay Hunt syndrome to whom the symptoms of facial nerve paralysis just emerged within several days) of a patient's face.
This study involved 56 patients diagnosed with Bell's palsy and Ramsay Hunt syndrome out of the patients with unilateral facial nerve palsy who had been referred to the rehabilitation medicine department for facial nerve conduction test from the otolaryngology department at Wonju Christian Hospital during the period of January 2009 to February 2011. Patients were excluded if they had a cardiac pacemaker, a history of facial nerve palsy, of seizure disorders, of traumatic brain damage or of stroke. The diagnosis of the 2 diseases was conducted by an experienced otolaryngologist, while all the subjects underwent facial nerve conduction testing and transcranial magnetic stimulation testing within 7 days of developing facial nerve palsy. The degree of facial nerve palsy was assessed using House-Brackmann facial grading scale (H-B FGS) [17].
Facial nerve conduction tests were conducted with Keypoint (Medtronic Inc., Minneapolis, MN, USA) and transcranial magnetic stimulation tests were performed using MagPro (Medtronic Inc.) while the patients were comfortable and relaxed. Facial nerve conduction tests were performed with supramaximal stimulation after the stimulator was placed at the stylomastoid foramen at a constant current with stimulation interval of 0.2 ms. To record compound muscle action potentials, the active electrode was set at the nasalis muscle while the reference electrode at the nasal bone in the opposite, employing the surface electrode. Latent phase was measured by the interval from the baseline to the onset point of initial negative peak [16]. Amplitudes were measured by the magnitude from the baseline to the negative peak of compound muscle action potentials [13,14].
When performing transcranial magnetic stimulation tests, the proximal part of the facial nerve was stimulated using a 9-cm diameter encircling coil rather than a labyrinthine segment. The strength of magnetic stimulation was increased during stimulation from 50% of the maximal stimulus for the healthy side and the affected side up to the maximal amplitude of compound muscle action potentials. For stimulus points, we moved the stimulator, starting from the parieto-occipital area to the occipital area, to spot promising regions that appeared to show the most rapid latent period.
A surface electrode was used to track compound muscle action potentials; the active electrode was recorded at the orbicularis oris muscle and the reference electrode was placed at the mandibular bone. Facial nerve conduction testing and transcranial magnetic stimulation testing were applied to both the healthy side and the affected side, comparing the amplitude differences in compound muscle action potentials between the 2 groups. Denervation ratio is defined as follows:
Denervation ratio=(healthy side amplitude-affected side amplitude)/healthy side amplitude×100
For statistical analysis, SPSS ver. 12.0 (SPSS Inc., Chicago, IL, USA) was implemented using non-parametric statistics, because the percentage of patients with Ramsay Hunt syndrome was low of the 52 participating patients. A comparison of gender and age between the 2 groups was analyzed using the chi-square test and Wilcoxon two-sample test, respectively. In order to compare the results of facial nerve conduction testing and transcranial magnetic stimulation testing for each patient, we used the Wilcoxon signed-rank test, while conducting the paired t-test for scaling the differences in the amplitude of compound muscle action potentials on facial nerve conduction testing and transcranial magnetic stimulation testing, which was performed separately for both groups. Mann-Whitney test was employed to confirm whether the differential values in facial nerve conduction test and transcranial magnetic stimulation test. To correlate the amplitudes between the 2 groups, we conducted the Pearson correlation test. Spearman's rank correlation was used to determine the correlation of the nerve block rates between H-B FGS and either the facial nerve conduction test or the transcranial magnetic stimulation test. Data were analyzed using descriptive statistics (mean±standard deviation) and statistical significance level was set at p<0.05.
Overall, there were 42 Bell's palsy cases (23 males, 19 females) and 14 Ramsay Hunt syndrome cases (10 males, 4 females) among the 56 participating patients. The average age was 49.1±18.3 years (range, 14 to 82 years) for the former and 44.2±16.8 years (range, 25 to 70 years) for the latter. The difference in the ages of each group was not statistically significant (p=0.348). H-B FGS found that for the Bell's palsy cases there were none patients of H-B FGS grade I, 10 patients of grade II, 22 patients of grade III, 10 patients of grade IV, and no patients of grade V; for the Ramsay Hunt syndrome cases, H-B FGS found no patients of grade I, 2 patients of grade II, 9 patients of grade III, 2 patients of grade IV, and 1 patient of grade V (Table 1). Overall, patients received testing at 5.41±1.56 days on average, after initial onset of facial paralysis symptoms. There was no significant difference between time to testing between the 2 groups; Bell's palsy patients underwent testing 5.48±1.47 days from symptoms onset and Ramsay Hunt syndrome cases underwent testing 5.21±1.85 days after onset of symptoms. For those who received the testing within 3 days after the onset of paralysis symptoms, the number totaled 10 patients, 7 Bell's palsy patients and 3 Ramsay Hunt syndrome patients.
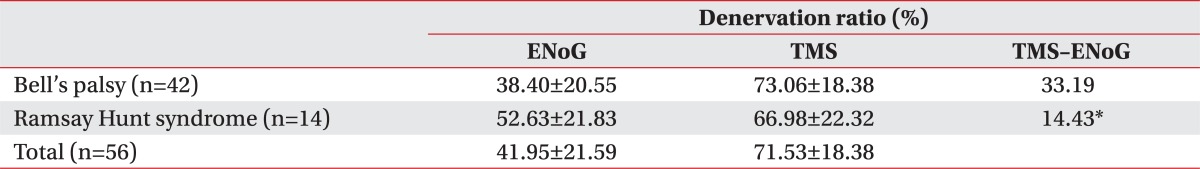
The overall nerve block rate on facial nerve conduction testing performed on the 56 patients turned out to be 41.95±21.59%. For the results in each group, the nerve block rate for Bell's palsy group was 38.40±20.55%, while 52.63±21.83% for Ramsay Hunt syndrome, which showed no statistical significance but a higher propensity of Ramsay Hunt syndrome group (p=0.057) (Table 2).
The nerve block rate of transcranial magnetic stimulation test on the overall patients was 71.53±18.38%. For the Bell's palsy group, the rate was 73.06±16.91%, while the rate was 66.98±22.32% for the Ramsay Hunt syndrome group. There was no statistically significant difference between the 2 groups in the rate of nerve blockings on transcranial magnetic stimulation test (p=0.389) (Table 2).
The nerve block rate of transcranial magnetic stimulation testing on the overall patients was found to be statistically significantly higher than that of facial nerve conduction testing (p<0.001). In addition, we saw a statistically significant difference in each group for the nerve block rates between the transcranial magnetic stimulation test and the facial nerve conduction test. The difference in the nerve block rates between the 2 tests led to determining the difference in the nerve block rates between the 2 tests to be lower in the Ramsay Hunt syndrome group than in the Bell's palsy group (p<0.001) (Table 2).
From the results of Pearson correlation index determined after creating the variables of age applied to the nerve block rate of facial nerve conduction testing, transcranial magnetic stimulation testing, and H-B FGS, there was a statistically significant difference found between the 2 groups that revealed a significant correlation in the nerve block rates between facial nerve conduction testing and transcranial magnetic stimulation testing (p<0.001). On the other hand, there was no statistically significant correlation between H-B FGS and nerve block rates of either of the 2 tests (Table 3).
Anatomically, the facial nerve constitutes 80% of the labyrinthine segment. Any inflammation or edema of this area in acute facial palsy patients is thought to lead to swelling of the facial nerve, which may develop a temporary block of nerve conduction or axonotmesis causing Wallerian degeneration. Conduction block or axonotmesis in Bell's palsy patients, as takes place in the medial temporal bone, the upper part of stylomastoid foramen at which electrical stimulation is to be conducted at facial nerve conduction test, is hard to confirm within 3 days immediately after symptom onset [18-21]. Also, the diagnosis of Ramsay Hunt syndrome at the first stage is difficult to make through facial nerve conduction test because the disease has its initial lesion at the geniculate ganglion as same as does Bell's palsy [6,22]. For Bell's palsy patients, on the other hand, motor-evoked potentials generated by transcranial magnetic stimulation, different from those measured by facial nerve conduction testing, remarkably decreased or disappeared in a few hours immediately after the development of the symptoms [13,14]. Also by transcranial magnetic stimulation test, conduction block or axonotmesis of the facial nerve for Ramsay Hunt syndrome patients can be detected in its initial phase, because these tests show pathophysiological and electrodiagnostic signs similar to those of Bell's palsy [16].
Nowak et al. [16], who performed research on 70 patients with facial palsy whose symptoms were detected within 3 days after symptom onset, maintained that the lower rate of compound muscle action potentials on facial nerve conduction testing was more significant in the Ramsay Hunt syndrome patients than in the Bell's palsy patients; these findings seemed to be responsible for more rapid and serious axonal damage in Ramsay Hunt syndrome patients than in Bell's palsy patients. Peitersen's research [23] confirmed a more unfavorable prognosis with Ramsay Hunt syndrome patients than for Bell's palsy patients. The present case showed that there was no statistical significance in the nerve block rates of facial nerve conduction test between the 2 groups; however, the nerve block rate increased considerably in the Ramsay Hunt syndrome cases, while there was no statistically significant difference found between the 2 groups in the nerve block rates on transcranial magnetic stimulation testing. However, the differences between the nerve block rates of the 2 tests, that is, the values earned by subtracting the nerve block rate of facial nerve conduction test from that of transcranial magnetic stimulation test, decreased significantly, which suggested that axonal injury progressed more rapidly in the Ramsay Hunt syndrome patients than in the Bell's palsy patients.
There has been a research result that long-term recovery rate of Bell's palsy patients was found unsatisfactory when its initial phase involved serious facial paralysis or when the denervation rate on facial nerve conduction test performed after its incidence reached more than 90% [24]. In addition, if we distinguish incomplete paralysis from complete paralysis based on the clinical standards, 94% of incomplete palsy patients and 61% of complete palsy patients recovered full function in the case of Bell's palsy, whereas for Ramsay Hunt syndrome only 66% of incomplete palsy patients and 10% of complete palsy patients were restored to full function, both altogether showing synkinesis [23,25]. Nowak et al. [16] argued that the degrees of facial paralysis and the decrement in the amplitudes on facial nerve conduction test measured within 3 days right after the onset of the palsy were correlated quantitatively to each other in patients with Bell's palsy (r2=0.70) and those with Ramsay Hunt syndrome (r2=0.66). In the present case, we tried to determine the relevance of H-B FGS to the nerve block rates on transcranial magnetic stimulation testing and on facial nerve conduction testing performed within 7 days of symptoms onset, but failed to find any statistically significant correlation. Comparing the present patient subjects with those in the previous studies, we suspect this was caused by the fact that the differences in the degrees of facial paralysis in our case were not diverse enough.
However, the nerve block rates on facial nerve conduction testing and transcranial magnetic stimulation testing showed a strong correlation to one another in both groups. Then, it is thought that performing a transcranial magnetic stimulation test within the first few days after symptom onset should be beneficiary towards making a prognosis for patients. On the contrary, a transcranial magnetic stimulation test 3 days or more after symptom onset may depreciate the diagnostic accuracy because of the progression of axonotmesis [20]. Because comparing the results of transcranial magnetic stimulation testing and facial nerve conduction testing helps in the diagnosis and prognosis of Bell's palsy and Ramsay Hunt syndrome, performing transcranial magnetic stimulation testing along with facial nerve conduction testing, to determine the progress rate and degree of lesions are expected to be useful towards making diagnoses and early prognostic predictions.
In conclusion, the present study has shown that for Ramsay Hunt syndrome and Bell's palsy transcranial magnetic stimulation test performed within the first few days after the onset of facial palsy has a high diagnostic value, correlated significantly with facial nerve conduction test. By comparing the results from transcranial magnetic stimulation testing and facial nerve conduction testing, we confirmed that axonotmesis injuries progress more rapidly in patients with Ramsay Hunt syndrome than in patients with Bell's palsy. These results seem to be beneficiary enough to help make the differential diagnosis of Bell's palsy and Ramsay Hunt syndrome, contributing to the ability to make prognostic predictions and treatment plans for patients. In the case of performing electrophysiologic testing to assess the facial nerve activity of patients with acute facial palsy, it is recommended to conduct facial nerve conduction tests along with transcranial magnetic stimulation tests for additional information about the neurophysiological status of a patient's facial nerve. By carrying out follow-up checks on patients with facial palsy, it is henceforth necessary to perform further studies in order to confirm how much the transcranial magnetic stimulation test could be useful in making prognostic predictions.
References
1. Atolini N Jr, Jorge JJ Jr, Gignon Vde F, Kitice AT, de Almeida Prado LS, Santos VG. Facial nerve palsy: incidence of different ethiologies in a tertiary ambulatory. Int Arch Otorhinolaryngol 2009;13:167-171.
2. Finsterer J. Management of peripheral facial nerve palsy. Eur Arch Otorhinolaryngol 2008;265:743-752. PMID: 18368417.



3. Robillard RB, Hilsinger RL Jr, Adour KK. Ramsay Hunt facial paralysis: clinical analyses of 185 patients. Otolaryngol Head Neck Surg 1986;95(3 Pt 1): 292-297. PMID: 3108776.


4. Takasu T, Furuta Y, Sato KC, Fukuda S, Inuyama Y, Nagashima K. Detection of latent herpes simplex virus DNA and RNA in human geniculate ganglia by the polymerase chain reaction. Acta Otolaryngol 1992;112:1004-1011. PMID: 1336296.


5. Furuta Y, Takasu T, Sato KC, Fukuda S, Inuyama Y, Nagashima K. Latent herpes simplex virus type 1 in human geniculate ganglia. Acta Neuropathol 1992;84:39-44. PMID: 1323906.


6. Murakami S, Mizobuchi M, Nakashiro Y, Doi T, Hato N, Yanagihara N. Bell palsy and herpes simplex virus: identification of viral DNA in endoneurial fluid and muscle. Ann Intern Med 1996;124(1 Pt 1): 27-30. PMID: 7503474.


7. Yanagihara N, Honda N, Hato N, Murakami S. Edematous swelling of the facial nerve in Bell's palsy. Acta Otolaryngol 2000;120:667-671. PMID: 11039881.


8. Fisch U, Esslen E. Total intratemporal exposure of the facial nerve: pathologic findings in Bell's palsy. Arch Otolaryngol 1972;95:335-341. PMID: 5018255.


9. Gantz BJ, Gmur A, Fisch U. Intraoperative evoked. electromyography in Bell's palsy. Am J Otolaryngol 1982;3:273-278. PMID: 7149140.


10. Yeo SW, Lee DH, Jun BC, Chang KH, Park YS. Analysis of prognostic factors in Bell's palsy and Ramsay Hunt syndrome. Auris Nasus Larynx 2007;34:159-164. PMID: 17055202.


11. Thomander L, Stalberg E. Electroneurography in the prognostication of Bell's palsy. Acta Otolaryngol 1981;92:221-237. PMID: 7324892.


12. May M, Blumenthal F, Klein SR. Acute Bell's palsy: prognostic value of evoked electromyography, maximal stimulation, and other electrical tests. Am J Otol 1983;5:1-7. PMID: 6881304.
13. Glocker FX, Magistris MR, Rosler KM, Hess CW. Magnetic transcranial and electrical stylomastoidal stimulation of the facial motor pathways in Bell's palsy: time course and relevance of electrophysiological parameters. Electroencephalogr Clin Neurophysiol 1994;93:113-120. PMID: 7512917.


14. Rosler KM, Magistris MR, Glocker FX, Kohler A, Deuschl G, Hess CW. Electrophysiological characteristics of lesions in facial palsies of different etiologies: a study using electrical and magnetic stimulation techniques. Electroencephalogr Clin Neurophysiol 1995;97:355-368. PMID: 8536586.


15. Rimpilainen I, Karma P, Laranne J, Eskola H, Hakkinen V. Magnetic facial nerve stimulation in Bell's palsy. Acta Otolaryngol 1992;112:311-316. PMID: 1604998.


16. Nowak DA, Linder S, Topka H. Diagnostic relevance of transcranial magnetic and electric stimulation of the facial nerve in the management of facial palsy. Clin Neurophysiol 2005;116:2051-2057. PMID: 16024292.


17. House JW, Brackmann DE. Facial nerve grading system. Otolaryngol Head Neck Surg 1985;93:146-147. PMID: 3921901.


18. Michaels L. Histopathological changes in the temporal bone in Bell's palsy. Acta Otolaryngol Suppl 1990;470:114-117. PMID: 2239225.


19. Podvinec M. Facial nerve disorders: anatomical, histological and clinical aspects. Adv Otorhinolaryngol 1984;32:124-193. PMID: 6369948.


20. Gilliatt RW, Taylor JC. Electrical changes following section of the facial nerve. Proc R Soc Med 1959;52:1080-1083. PMID: 13850113.

21. Mamoli B. Prognostic assessment in peripheral facial nerve paralysis with particular reference to electroneurography. Wien Klin Wochenschr Suppl 1976;53:3-28. PMID: 181919.

22. Furuta Y, Takasu T, Fukuda S, Sato-Matsumura KC, Inuyama Y, Hondo R, et al. Detection of varicella-zoster virus DNA in human geniculate ganglia by polymerase chain reaction. J Infect Dis 1992;166:1157-1159. PMID: 1328403.



23. Peitersen E. Bell's palsy: the spontaneous course of 2,500 peripheral facial nerve palsies of different etiologies. Acta Otolaryngol Suppl 2002;(549): 4-30. PMID: 12482166.


24. Mantsopoulos K, Psillas G, Psychogios G, Brase C, Iro H, Constantinidis J. Predicting the long-term outcome after idiopathic facial nerve paralysis. Otol Neurotol 2011;32:848-851. PMID: 21659930.


25. Devriese PP, Moesker WH. The natural history of facial paralysis in herpes zoster. Clin Otolaryngol Allied Sci 1988;13:289-298. PMID: 2846216.