- Search
| Ann Rehabil Med > Volume 46(3); 2022 > Article |
|
Abstract
Objective
To compare the predicted and actual maximal heart rate (HRmax) values in the cardiopulmonary exercise test (CPET).
Methods
We retrospectively investigated 1,060 patients who underwent a CPET between January 2016 and April 2020 at our institution’s cardiopulmonary rehabilitation center. The following patients were included: those aged >20 years, those tested with a treadmill, and those who underwent symptom-limited maximum exercise testing— reaching ≥85% of the predicted HRmax (62% if taking beta-blockers) and highest respiratory exchange ratio ≥1.1. Ultimately, 827 patients were included in this study. Data on diagnosis, history of taking beta-blockers, age, body mass index (BMI), and CPET parameters were collected. Subgroup analysis was performed according to age, betablockers, BMI (low <18.5 kg/m2, normal, and high ≥25 kg/m2), and risk classification.
Results
There was a significant difference between the actual HRmax and the predicted value (p<0.001). Betablocker administration resulted in a significant difference in the actual HRmax (p<0.001). There were significant differences in the moderate-to-high-risk and low-risk groups and the normal BMI and high BMI groups (p<0.001). There was no significant difference between the elderly and younger groups. We suggest new formulae for HRmax of cardiopulmonary patients: estimated HRmax=183-0.76×age (the beta-blocker group) and etimated HRmax=210-0.91×age (the non-beta-blocker group).
An adequate exercise intensity must be determined to prescribe exercise for patients with cardiopulmonary diseases. Heart rate increases in proportion to exercise intensity and is an indicator used to set the exercise intensity [1-3]. Resting heart rate (HR) and maximal heart rate (HRmax) must be first evaluated by conducting a cardiopulmonary exercise test (CPET) to determine the target heart rate during exercise [4,5]. However, a CPET requires costly equipment, space, and skilled examiners, which are not readily available in every hospital [6].
In such cases, predicted HRmax may be used. Aging leads to decreased physiological functions and HRmax. Accordingly, HRmax is estimated using age. In clinical settings, HRmax=220-age [7] is widely used [8]. However, this formula had serious limitations [9]. This formula was developed based on 11 references with small sample sizes. A recent study also questioned the limitations of this formula [10]. Therefore, many researchers presented an alternative formula to calculate HRmax using data of large sample size: 206.3-0.711×age [11] and 217-0.85×age [12].
However, these estimated formulas still have considerations. All the above papers estimated HRmax for healthy college-aged participants. However, patients with cardiopulmonary disease may have different hemodynamic responses. In addition, the number of patients aged over 70 years is gradually increasing, and their hemodynamic response may be different from that of younger patients [13]. However, there is a lack of studies on the feasibility of previously developed HRmax estimation in patients with cardiopulmonary diseases.
Therefore, this study retrospectively analyzed CPET data of cardiopulmonary patients to see if the existing prediction method of HRmax could reflect the actual HRmax, as it is extremely important for appropriate exercise prescriptions.
This was a single-center retrospective study that analyzed the medical records of 1,060 patients. This study was approved by the Institutional Review Board of Pusan National University Hospital (No. 2109-020-107). The informed consent was waived due to retrospective study.
We investigated 1,981 records of 1,060 patients who performed a CPET from January 2016 to April 2020 at our institution’s cardiopulmonary rehabilitation center. When a patient performed the test several times, the record with the highest peak respiratory exchange ratio (RER) value was adopted because it was judged that sufficient exercise was performed. A total of 719 male and 341 female patients aged between 15 and 87 years were included. All participants underwent clinical examination by a physician. Before a CPET, the history of medications such as the use of beta-blockers, antiplatelet agents, angiotensinconverting enzyme inhibitors, diuretics, and statins was investigated and inserted into the CPET result sheet.
The following patients were included in this study: (1) patients diagnosed with cardiopulmonary disease, (2) patients aged over 20 years, (3) patients who performed a CPET using a treadmill, and (4) patients who underwent a symptom-limited maximal exercise test—i.e., symptom-limited maximum exercise testing was defined as reaching more than 85% of the predicted HRmax (62% if taking beta-blockers [14-16]) and RER of ≥1.1.
As the test was conducted on patients with cardiopulmonary diseases, certain tests were terminated early for different reasons, and the heart rate could not be accurately measured due to arrhythmia. Data of patients who satisfied the following were excluded to include only the data of those who appropriately performed maximum exercise testing: (1) those who failed to reach 85% of the predicted HRmax (62% if on beta-blockers), (2) patients with the highest RER of <1.1, (3) patients with an abnormal heart rate response due to arrhythmia, (4) patients under the age of 20 years, and (5) patients whose HRmax was measured using an ergometer.
CPET using a CASE Treadmill (GE Healthcare, Chicago, IL, USA) was performed using either the modified Bruce protocol or Naughton protocol, according to the physical function of the patients. The test was terminated when the patient became physically exhausted from maximal exercise or met the discontinuation criteria according to the American Thoracic Society. Oxygen intake (VO2) and carbon dioxide emission (VCO2) during exercise were assessed by the breath-by-breath method using a Quark-CPET gas analyzer (COSMED, Albano Laziale, Rome, Italy). The collected gas was then used to evaluate the peak oxygen uptake (VO2peak), RER, and minute ventilation-carbon dioxide production relationship slope (VE/VCO2 slope). Twelve-lead electrocardiograms (CASE, GE Healthcare) were recorded during the pre-exercise phase, exercise phase, and up to 5 minutes in the recovery phase. Blood pressure and HR were measured using a Tango M2 sphygmomanometer (Suntech-Medical, Morrisville, NC, USA) during each phase. Rating of perceived exertion (RPE) was evaluated during each stage. HRmax was measured to assess whether 85% of the predicted HRmax was reached (62% for patients on beta-blockers). After performing maximum exercise and stopping, a cool-down period of 5 minutes was given.
Patients were grouped according to their characteristics. The patients were divided into two groups based on their age. Patients aged over 70 years were defined as the elderly group. Patients were also divided into the cardiac and pulmonary disease groups. In the cardiac and pulmonary disease groups, patients were classified according to the severity of the disease using the American Association of Cardiovascular and Pulmonary Rehabilitation (AACVPR) guidelines and Michele’s criteria, respectively [17].
Patients with a body mass index (BMI) of <18.5 kg/m2, 18.5–25 kg/m2, and ≥25 kg/m2 were classified into the underweight, normal, and overweight groups, respectively. By examining the history of the drug being taken, the patients were divided into two groups according to whether they were taking beta-blockers.
A total of 827 patients were included in the final analysis, and the baseline characteristics of the participants are shown in Table 1.
Descriptive statistics of continuous variables are presented as the mean and standard deviation (SD). Linear regression models were used to determine the association between HRmax and age. All possible sub-models were fit. The best model was selected according to Mallows’ Cp statistic. This method, which takes into consideration the number of possible predictor variables, allows one to select the model that best fits the data.
Approximate residual normality and homoscedasticity were also checked. Prediction intervals from this model were compared with the actual HRmax with the HRmax=220-age. A p-value of <0.05 was considered statistically significant.
We used the independent t-test to analyze the participants’ characteristics and the chi-square test to compare based on the BMI and risk classification between groups. Within and between groups, the effect of beta-blockers was analyzed by one-way analysis of variance (ANOVA). We used the Bonferroni correction and least significant difference (LSD) to perform multiple post-hoc tests. The significance level was set at p<0.05. All statistical tests were performed using SPSS version 22.0 for Windows (IBM, Armonk, NY, USA).
CPET data of 827 patients were analyzed. The mean age of the participants was 60.29±12.63 years, and 570 participants (68.9%) were males. Among the participants, 207 (25.0%) belonged to the elderly group. Actual HRmax measured through testing varied from 91 to 199 beats per minute (bpm) with a mean±SD of 146.56±20.46 bpm. Predicted HRmax predicted using HRmax=220– age ranged between 133 and 200 bpm with a mean±SD of 159.71±12.63 bpm. Actual HRmax was significantly lower than the predicted HRmax in all participants (p<0.001), and there was no difference according to age (Table 2, Fig. 1).
A total of 396 participants (47.9%) were taking betablockers. HRmax was significantly lower in the betablocker group than in the non-beta-blocker group (137.97±21.06 vs. 154.46±16.30, p<0.001). It was the same in each subgroup (Table 3). As shown in Fig. 2, the results were plotted on scatterplots used to derive new equations predicting the actual HRmax. Depending on whether beta-blockers were taken, two equations were derived (estimated HRmax=183-0.76×age in the beta-blocker group, 210-0.91×age in the non-beta-blocker group) (Fig. 2).
Among all participants, 537 (64.9%) were in the cardiac disease group and 290 (35.1%) were in the pulmonary disease group, respectively. The most common cardiac disease was acute coronary syndrome (62.8%), and the most common pulmonary disease was lung cancer (62.4%). In both groups, the actual HRmax was significantly lower than the predicted HRmax (p<0.001 for both groups).
There were 492, 25, and 310 patients in the normal BMI, low BMI, and high BMI groups, respectively. In the betablocker group, the actual HRmax was significantly lower than the predicted HRmax in all groups (p<0.05). In particular, in the beta-blocker group, a significant difference between the actual HRmax and the predicted HRmax was confirmed between the normal BMI and high BMI groups (Table 4).
A total of 371 (44.9%), 364 (44.0%), and 92 (11.1%) participants were classified into the low-, moderate-, and high-risk group, respectively. The difference between the actual HRmax and predicted HRmax was significant in all risk groups, and the difference was smaller in the lowrisk group than in the moderate- and high-risk groups (p<0.001).
The primary goal of this study was to confirm whether the predicted HRmax using HRmax=220-age was reliable in patients with cardiopulmonary diseases. The secondary goal was to determine whether, in addition to age, beta-blocker use, health condition, and disease severity affected HRmax prediction.
Here, we observed that there was a difference of ≥10 bpm between the predicted HRmax and actual HRmax. The different was not only statistically but also clinically significant. A difference of 10 bpm in the heart rate in the exercise prescription is equivalent to an exercise intensity of 1 MET (metabolic equivalent of task). This suggests that higher-intensity exercise that is not adequate for patients may be prescribed. It is essential to measure actual HRmax by performing a CPET when prescribing exercise for patients in need of cardiopulmonary rehabilitation. However, when a CPET cannot be conducted, and the HRmax needs to be predicted, the use of HRmax=220-age may cause an over-estimation of the target heart rate. This was observed in the scatter plot of the actual HRmax and age. It was confirmed that beta-blocker administration had a significant effect on the HRmax during a CPET. If it is possible to know whether a patient is on betablockers, it would be good to selectively apply these two HRmax prediction formulas (predicted HRmax=183-0.76×age in the beta-blocker group, 210-0.91×age in the non-beta-blocker group).
There was no difference in the chronotropic response to exercise in patients aged over 70 years. In the two groups divided by age, the actual HRmax was approximately 92% of the predicted HRmax, and the SD was not different between the two groups. This suggests that age is not a barrier to exercise. To the best of our knowledge, this study is the first to derive a formula for predicting the HRmax in elderly patients with cardiopulmonary diseases.
In addition to age, other factors that may affect the hemodynamic response in patients were analyzed. First, the clinically known risk classification was analyzed. The risk of exercise in patients with cardiac disease was evaluated according to the AACVPR Stratification Algorithm for Risk of Event. Risk was classified into high, moderate, and low based on the medical history, cardiac function, type of procedures or surgeries, and cardiopulmonary exercise capacity of patients. Most patients with pulmonary disease in our study had lung cancer and underwent a CPET to confirm preoperative and postoperative cardiopulmonary function. These patients were classified based on the risk stratification of Salati et al. [17], which classifies the possibility of life-threatening complications after lung resection in early-stage lung cancer. As both risk classification methods are clinical classifications to predict prognosis, the methods were analyzed together. The one-way ANOVA test, Bonferroni and LSD corrections showed that the difference between the actual HRmax and predicted HRmax was significant between low risk and moderate-to-high risk. In other words, a higher risk was associated with a lower actual HRmax than predicted HRmax, and this suggests the use of the current formula may overestimate HRmax, which may be dangerous for the patients. Therefore, predicted HRmax may be used to prescribe exercise in low-risk patients; however, in highrisk patients with cardiopulmonary diseases, the actual HRmax needs to be assessed through a CPET for safety reasons.
Patients were divided into groups according to their BMI. There was a significant difference between the three BMI groups among the participants taking beta-blockers in the one-way ANOVA. In the Bonferroni correction, the difference between the predicted and actual HRmax between the normal and high BMI groups was significant. There was no significant difference between the groups not taking beta-blockers. It is thought that this is because there were many patients with cardiac disease in the beta-blocker group, with a higher BMI. Obesity is associated with a shortened lifespan and significantly increases the risk of cardiovascular morbidity and mortality compared with a normal BMI [18]. The non-beta-blocker group had a relatively high proportion of patients with pulmonary disease. Patients with chronic obstructive pulmonary disease (COPD) and lung cancer account for a large number, and among these patients, there are studies on the “obesity paradox” that individuals with a high BMI show a significantly better long-term survival rate [19,20].
In summary, the difference between the predicted and actual HRmax was large in patients with a higher risk for cardiopulmonary rehabilitation and abnormal BMI. This indicated that the HRmax values of such patients are challenging to predict. This may be because patients with more severe diseases are more likely to end the CPET earlier than those with less severe diseases. However, the actual HRmax tended to be lower than the predicted HRmax even in patients who appropriately performed the CPET in this study. In patients with severe cardiopulmonary diseases, the predicted HRmax without a CPET may cause more intense exercises to be prescribed, which could be alarming for the patients.
Several limitations must be considered while interpreting the results of this study. First, this was a single-center study that does not represent all patients with cardiopulmonary diseases in South Korea. However, compared with the findings of previous studies, VO2peak and HRmax were similar, suggesting that our results were reliable [5]. In the future, a large-scale multicenter study must be conducted to present representative data for Koreans.
Second, heart rate cannot be predicted for all types of exercise. CPET results using an ergometer were not included in this study. Compared with exercise using a treadmill, those using an upper or lower extremity ergometer show a significant difference in the physiological response [21]. Exercise with an ergometer is known to have a lower heart rate compared with exercise using a treadmill [22]. However, in this study, analysis was not possible due to the small number of patients who underwent a CPET using an ergometer. Further studies are needed in patients with paraplegia due to spinal cord injury and in patients using wheelchairs or walkers due to lower extremity amputation.
Third, among patients, especially the elderly, only those with the ability to perform a CPET were included; therefore, it was challenging to apply the formula to the elderly who found it difficult to perform a CPET. This may have led to a selection bias. However, for such patients, rather than a program to set the target heart rate and reach the intensity, exercise prescriptions are being administered at the clinic focusing on increasing basic lower extremity strength, balance, walking ability, and endurance. This formula should be applied selectively.
In conclusion, our study showed that there is a significant difference between the actual HRmax and predicted HRmax calculated using HRmax=220-age. It was also confirmed that the difference may vary depending on whether beta-blockers were taken. Herein, we propose a new formula (predicted HRmax=183-0.76×age in the beta-blocker group, 210-0.91×age in the non-beta-blocker group), that has been constructed based on the actual HRmax in patients with cardiopulmonary diseases. For patients previously diagnosed as having low risk, exercise prescription can be possible with this formula alone. However, high-risk groups or obese patients have a large difference between the predicted and actual HRmax. Thus, it is recommended that a CPET is performed as much as possible for appropriate exercise prescription.
AUTHOR CONTRIBUTION
Conceptualization: Lee BJ, Shin YB. Methodology: Han SH, Lee BJ, Shin YB. Formal analysis: Kim YM, Choi MS. Funding acquisition: Kim YM, Kim SH. Project administration: Han SH, Kim DM. Visualization: Park HE, Choi MS, Kim DM. Writing – original draft: Han SH, Hong JW, Lee BJ. Writing – review and editing: Kim SH, Shin YB, Lee BJ. Approval of final manuscript: all authors.
Fig. 1.
Comparison of actual maximal heart rate (HR) and age-predicted maximal HR. Boxplots of (A) beta-blocker group (n=431) and (B) non-beta-blocker group (n=431). Participants were divided into subgroups according to age, body mass index (BMI, kg/m2), and risk classification. *p<0.05 (Bonferroni correction for continuous variable), **p<0.05 (least significant difference correction for continuous variable).
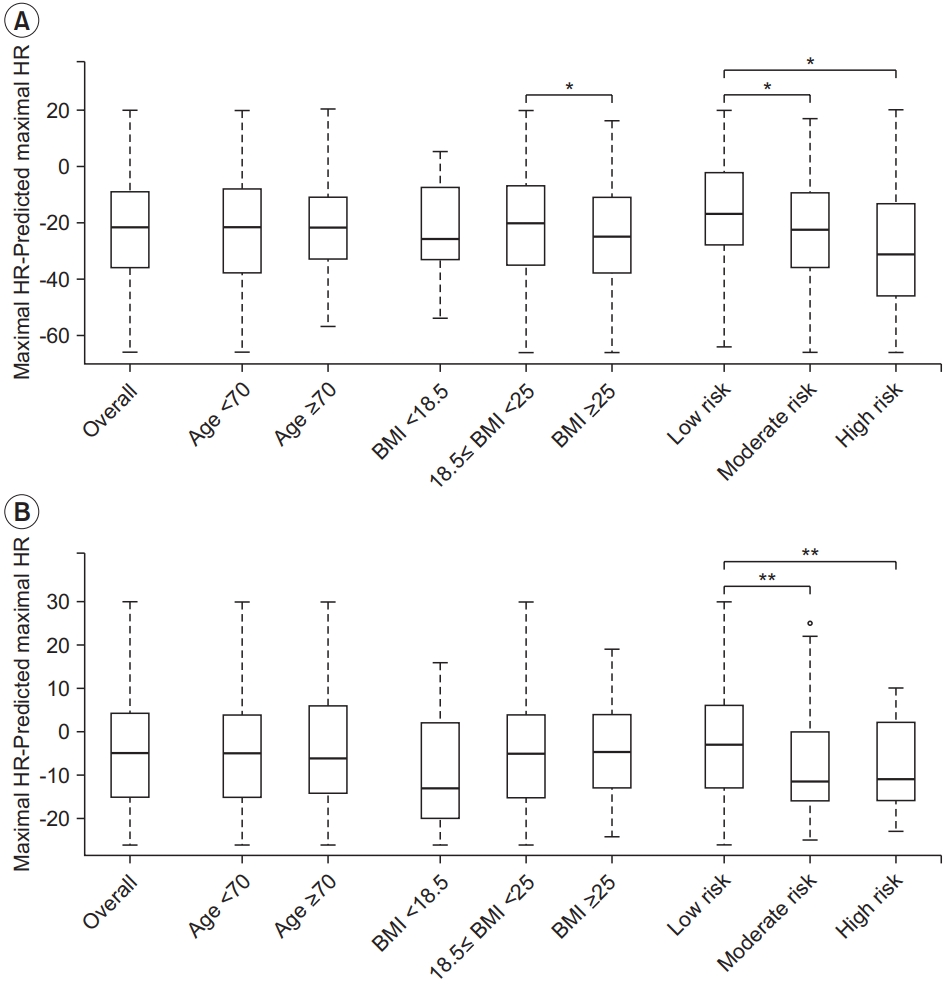
Fig. 2.
Scatterplot between age and actual maximal heart rate (n=827). Divided into two groups depending on whether they were taking beta-blockers or not. (A) Group with taking beta-blockers (n=396). (B) Group without betablockers (n=431). And divided into by disease group, (C) cardiac disease group (n=537) and (D) pulmonary disease group (n=290). All participants were classified into high risk, moderate risk, and low risk according to the risk classification and displayed in different diagrams.
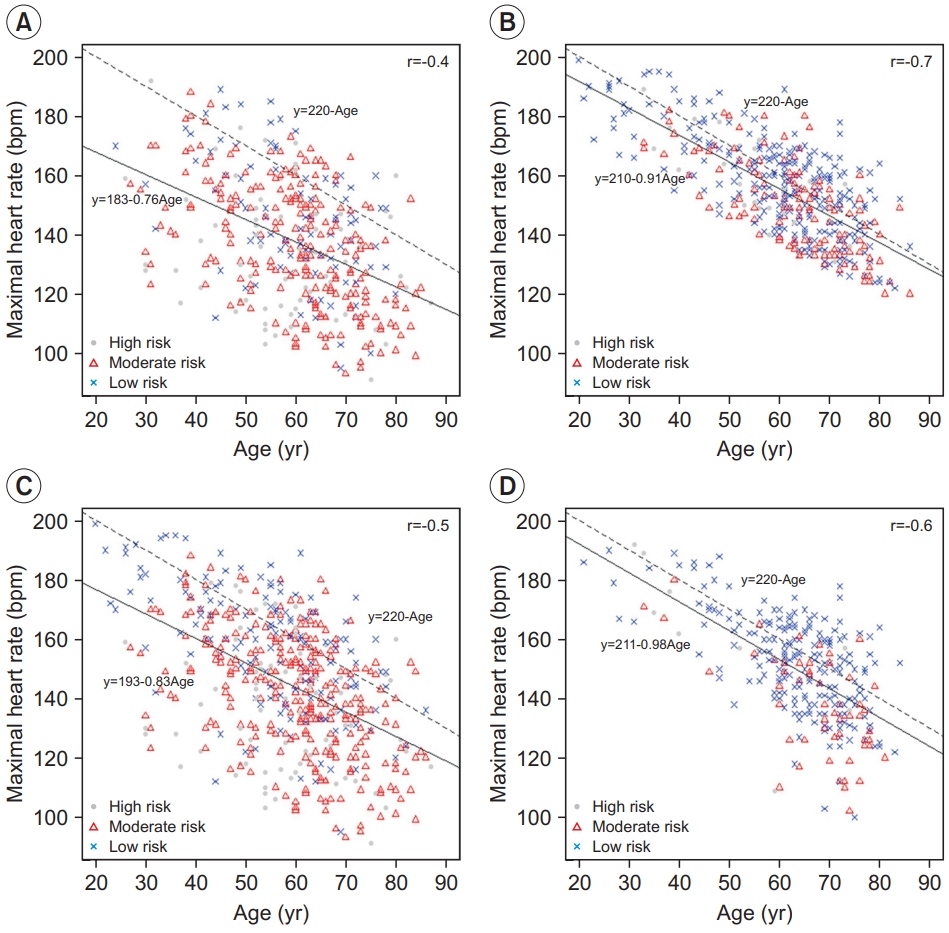
Table 1.
Baseline characteristics of the patients (n=827)
Table 2.
Comparison of the beta-blocker group and non-beta-blocker group
| Factor | Beta-blocker group (n=396) | Non-beta-blocker group (n=431) | p-value |
|---|---|---|---|
| Sex | |||
| Male | 298 (75.3) | 272 (63.1) | |
| Female | 98 (24.7) | 159 (36.9) | |
| Age (yr) | 59.56±12.47 | 60.97±12.76 | 0.109 |
| <70 | 306 (77.3) | 314 (72.9) | 0.166 |
| ≥70 | 90 (22.7) | 117 (27.1) | |
| BMI (kg/m2) | 24.90±3.40 | 23.70±2.89 | <0.001* |
| <18.5 | 8 (2.0) | 17 (3.9) | <0.001* |
| 18.5–25 | 214 (54.0) | 278 (64.5) | |
| ≥25 | 174 (43.9) | 136 (31.6) | |
| Actual HRmax (bpm) | 137.97±21.06 | 154.46±16.30 | <0.001* |
| Predicted HRmax (bpm) | 160.44±12.47 | 159.03±12.76 | 0.109 |
| Risk classification | <0.001* | ||
| Low risk | 93 (23.5) | 278 (64.5) | |
| Moderate risk | 236 (59.6) | 128 (29.7) | |
| High risk | 67 (16.9) | 25 (5.8) |
Table 3.
Comparison of the actual HRmax between the beta-blocker group and non-beta-blocker group by the physiological variables
| Factor |
Beta-blocker group |
Non-beta-blocker group |
p-value | ||
|---|---|---|---|---|---|
| n | Actual HRmax | n | Actual HRmax | ||
| Age (yr) | |||||
| <70 | 306 | 141.89±20.51 | 314 | 158.91±15.13 | <0.001* |
| ≥70 | 90 | 124.63±17.15 | 117 | 142.50±13.02 | <0.001* |
| BMI (kg/m2) | |||||
| <18.5 | 8 | 135.25±16.15 | 17 | 150.29±17.85 | <0.001* |
| 18.5–25 | 214 | 139.04±20.32 | 278 | 155.17±16.63 | <0.001* |
| ≥25 | 174 | 136.77±22.15 | 136 | 153.53±15.40 | <0.001* |
| Risk classification | |||||
| Low risk | 93 | 144.86±21.07 | 278 | 156.73±16.37 | <0.001* |
| Moderate risk | 236 | 136.68±20.52 | 128 | 149.07±15.06 | <0.001* |
| High risk | 67 | 132.93±20.93 | 25 | 156.80±15.84 | <0.001* |
| Disease group | |||||
| Cardiac disease | 360 | 138.78±20.96 | 177 | 158.02±17.12 | <0.001* |
| Pulmonary disease | 36 | 129.81±20.64 | 254 | 151.98±15.26 | <0.001* |
Table 4.
Comparison of actual HRmax and age-predicted HRmax by physiologic variables
| HRmax | Predicted HRmax | Difference | |||
|---|---|---|---|---|---|
| Beta-blocker group | Age (yr) | <70 (n=306) | 141.89±20.51 | 164.98±10.26 | -23.09±19.61 |
| ≥70 (n=90) | 124.63±17.15 | 145.00±4.19 | -20.37±16.96 | ||
| p-value | <0.001* | <0.001* | 0.233 | ||
| BMI (kg/m2) | <18.5 (n=8) | 135.25±16.15 | 158.00±10.99 | -22.75±19.04 | |
| 18.5–25 (n=214) | 139.04±20.32 | 159.36±11.52 | -20.32±19.58a) | ||
| ≥25 (n=174) | 136.77±22.15 | 161.88±13.53 | -25.11±18.14a) | ||
| p-value | 0.536 | 0.121 | 0.048** | ||
| Risk classification | Low risk (n=93) | 144.86±21.07 | 160.67±11.62 | -15.81±18.50b) | |
| Moderate risk (n=236) | 136.68±20.52 | 159.89±12.46 | -23.20±17.70b) | ||
| High risk (n=67) | 132.93±20.93 | 162.09±13.62 | -29.16±21.67b) | ||
| p-value | 0.001** | 0.435 | <0.001** | ||
| Non-beta-blocker group | Age (yr) | <70 (n=314) | 158.91±15.13 | 164.09±11.13 | -5.18±11.26 |
| ≥70 (n=117) | 142.50±13.02 | 145.46±3.78 | -2.96±12.28 | ||
| p-value | <0.001* | <0.001* | 0.076 | ||
| BMI (kg/m2) | <18.5 (n=17) | 150.29±17.85 | 159.00±12.29 | -8.71±12.63 | |
| 18.5–25 (n=278) | 155.17±16.63 | 159.65±13.12 | -4.48±11.86 | ||
| ≥25 (n=136) | 153.53±15.40 | 157.79±12.04 | -4.26±10.80 | ||
| p-value | 0.355 | 0.379 | 0.320 | ||
| Risk classification | Low risk (n=278) | 156.73±16.37 | 159.69±13.28 | -2.97±11.68c) | |
| Moderate risk (n=128) | 149.07±15.06 | 156.49±11.31 | -7.42±11.01c) | ||
| High risk (n=25) | 156.80±15.84 | 164.72±11.39 | -7.92±9.99c) | ||
| p-value | <0.001** | 0.004** | <0.001** | ||
Values are presented as mean±standard deviation or number (%).
HRmax, maximal heart rate; BMI, body mass index; ANOVA, analysis of variance.
b) The following post-hoc analysis was performed using the Bonferroni correction: low-risk and moderate-risk (p=0.004), low-risk and high-risk (p=0.001), moderate-risk and high risk (p=0.573).
REFERENCES
1. Karvonen J, Vuorimaa T. Heart rate and exercise intensity during sports activities: practical application. Sports Med 1988;5:303-11.

2. Esposito F, Impellizzeri FM, Margonato V, Vanni R, Pizzini G, Veicsteinas A. Validity of heart rate as an indicator of aerobic demand during soccer activities in amateur soccer players. Eur J Appl Physiol 2004;93:167-72.



3. Hills AP, Byrne NM, Ramage AJ. Submaximal markers of exercise intensity. J Sports Sci 1998;16 Suppl:S71-6.


4. Sebastian LA, Reeder S, Williams M. Determining target heart rate for exercising in a cardiac rehabilitation program: a retrospective study. J Cardiovasc Nurs 2015;30:164-71.

5. Albouaini K, Egred M, Alahmar A, Wright DJ. Cardiopulmonary exercise testing and its application. Postgrad Med J 2007;83:675-82.



6. Ozeki N, Fukui T, Iwano S, Hakiri S, Nakamura S, Kawaguchi K, et al. Factors associated with changes in the 12-m stair-climbing time after lung lobectomy. Gen Thorac Cardiovasc Surg 2021;69:282-9.



7. Fox SM 3rd, Naughton JP, Haskell WL. Physical activity and the prevention of coronary heart disease. Ann Clin Res 1971;3:404-32.


8. Sporis G, Vucetic V, Jukic I, Omrcen D, Bok D, Custonja Z. How reliable are the equations for predicting maximal heart rate values in military personnel? Mil Med 2011;176:347-51.


9. Lewis GD, Bossone E, Naeije R, Grunig E, Saggar R, Lancellotti P, et al. Pulmonary vascular hemodynamic response to exercise in cardiopulmonary diseases. Circulation 2013;128:1470-9.


10. Robergs RA, Landwehr R. The surprising history of the “HRmax=220-age” equation. J Exerc Physiol Online 2002;5:1-10.
11. Londeree BR, Moeschberger ML. Influence of age and other factors on maximal heart rate. J Cardiac Rehabil 1984;4:44-9.
12. Miller WC, Wallace JP, Eggert KE. Predicting max HR and the HR-VO2 relationship for exercise prescription in obesity. Med Sci Sports Exerc 1993;25:1077-81.

13. Strait JB, Lakatta EG. Aging-associated cardiovascular changes and their relationship to heart failure. Heart Fail Clin 2012;8:143-64.



14. Wonisch M, Hofmann P, Fruhwald FM, Kraxner W, Hodl R, Pokan R, et al. Influence of beta-blocker use on percentage of target heart rate exercise prescription. Eur J Cardiovasc Prev Rehabil 2003;10:296-301.


15. Kligfield P, Lauer MS. Exercise electrocardiogram testing: beyond the ST segment. Circulation 2006;114:2070-82.


16. Hong SP, Lee YS, Lee JB, Ryu JK, Choi JY, Kim KS. Prognostic value of heart rate reserve in exercise treadmill test after coronary revascularization. Intern Med 2014;4:175.

18. Khan SS, Ning H, Wilkins JT, Allen N, Carnethon M, Berry JD, et al. Association of body mass index with lifetime risk of cardiovascular disease and compression of morbidity. JAMA Cardiol 2018;3:280-7.



19. Li S, Wang Z, Huang J, Fan J, Du H, Liu L, et al. Systematic review of prognostic roles of body mass index for patients undergoing lung cancer surgery: does the ‘obesity paradox’ really exist? Eur J Cardiothorac Surg 2017;51:817-28.


20. Zewari S, Vos P, van den Elshout F, Dekhuijzen R, Heijdra Y. Obesity in COPD: revealed and unrevealed issues. COPD 2017;14:663-73.


- TOOLS







