- Search
| Ann Rehabil Med > Volume 44(1); 2020 > Article |
|
Abstract
We report two cases of postictal urinary retention in pediatric patients with cognitive impairment. Two girls with intellectual disabilities, concomitant cerebral palsy (case 1) and Rett syndrome (case 2), developed urinary retention following seizures. Their caregivers brought them to the hospital with complaints of abdominal distension. After excluding neurological progression, they were referred to the rehabilitation clinic for the evaluation and management of postictal urinary retention. We followed two different approaches in each case to restore normal urination. While serial manual cystometrograms were performed in case 1, clean intermittent catheterization with a voiding diary was performed in case 2 until restoration of normal urination. Based on these pediatric cases of successfully managed postictal urinary retention, we suggest that more attention may be needed for children with cognitive impairment to diagnose and manage postictal urinary retention.
Acute urinary retention is reported to affect 7–8 in 100,000 children visiting the emergency room with lower urinary tract symptoms [1]. There are various causes of acute urinary retention, but seizure as a cause has rarely been reported, and its incidence and clinical features have not been thoroughly elucidated in previous studies. Furthermore, guidelines for managing these symptoms have not been clearly reported to date [2].
Acute urinary retention may occur after the development of brain lesions. Even without mechanical destruction of brain tissue, loss of pontine micturition center function due to seizure can lead to urinary retention [3].
We report two pediatric cases of postictal urinary retention without acute structural brain lesions. We suggest the importance of recognizing the timing of symptom recovery and clarify the differences compared to that in adults. In particular, by reporting cases of functionally impaired children, we aimed to provide information concerning precautions related to intellectual and motor disabilities.
Written informed consents were obtained.
A 10-year-old girl was admitted to the pediatric department for abdominal distension, fever, and non-pitting edema with suspected acute urinary retention 4 days after a seizure. She was previously diagnosed with dystonic cerebral palsy, profound intellectual disability, and Lennox-Gastaut syndrome. Her mother reported that her urine output had markedly reduced during diaper changing compared to the period before the seizure. On the day of hospital admission, no urination was observed for 10 hours.
On the electroencephalograms (EEGs), frequent polyspike-wave complexes were noted over the frontal area. Plain X-ray of the abdomen showed no abnormal findings of abdominal distension. Urinalysis revealed positive results for urinary tract infection (UTI) and acute kidney injury (AKI).
Through immediate urethral catheterization, the urinary retention of 750 mL was resolved. Despite improvement of UTI while maintaining the indwelling catheter for 7 days, no urination was observed after removal of the catheter. She was referred to our rehabilitation clinic for evaluation of voiding difficulty and developing a care plan. We performed serial rounds of manual cystometrogram (CMG) in the supine position to maintain constant abdominal pressure, supposing that her maximal bladder capacity was 360 mL based on Koff’s formula. After the 4th round of CMG, which resulted in a pressure surge, we removed the indwelling catheter safely without any complications (Table 1).
A 6-year-old girl presented with relapsing febrile seizure sustained for 2 days. She was previously diagnosed with Rett syndrome with severe intellectual disability. During history taking, her mother remembered that she presented with intermittent lower abdominal distension and an overflow incontinence pattern that was observed 1 day before the admission.
Her EEGs revealed frequent, spike-and-wave discharges over both centro-temporoparietal areas. On routine abdominal X-ray, an abdominal mass was observed, which was later revealed to be a distended bladder (Fig. 1). Urinalysis revealed negative results for UTI and AKI. An indwelling urethral catheter was put in place, and the urinary retention was determined to be 1,000 mL, approximately 4 times the estimated maximal bladder capacity.
Although the seizures were controlled, urinary retention persisted. After self-voiding attempts were made with suprapubic tapping, clean intermittent catheterization (CIC) was performed 4–6 times per day to follow up on her post-void residual (PVR), along with voiding diaries. Subsequently, the frequency of CIC was reduced as the PVR decreased. On day 15, CIC was discontinued because the PVR was consistently less than 50 mL, indicating no urinary retention.
The initial management of acute urinary retention to preserve the upper urinary tract is the immediate decompression of the bladder [4]. However, the management and evaluation methods specific to postictal urinary retention are yet to be investigated.
Here, we report two pediatric cases of postictal urinary retention, in which the patients recovered normal urination without complications. We suggest that these cases may reflect transient postictal weakness, also known as Todd’s palsy.
The significance of this report is that there may be differences in the causes of acute urinary retention and risk of complications between adults and children. Furthermore, we suggest that CMG and CIC with voiding diaries can be used for uncooperative patients as alternatives to the traditional urodynamic study (UDS)-based evaluation used in cooperative patients to check for the recovery of bladder function, emphasizing some considerations regarding the underlying pathology of the patient.
With respect to the approach to manage acute urinary retention, there are some differences between adults and children. First, most cases of urinary retention in adults are caused by mechanical obstruction or as a side effect of medication; therefore, priority should be given to evaluating structural lesions that affect the urinary tract and investigating drug history [1,4]. In contrast, the incidence of neurological disorders is higher and functional recovery should be carefully observed while managing neurologic conditions in children. Secondly, according to Koff’s formula, only age acts as an independent variable in predicting bladder capacity. It may be inferred that children are more vulnerable to upper urinary tract complications with urinary retention than adults.
Furthermore, we focused on additional considerations owing to differences between healthy and disabled children. Limited fluid intake due to swallowing problems may lead to a bladder capacity deficit, and urinary continence is hardly maintained in severely mentally disabled and motor-impaired children [5]. Considering the nature of the underlying disease, children with cerebral palsy have delayed and incomplete development of the bladder. It means that they have reduced bladder capacity with uninhibited bladder contractions, which has potentially negative effects on the upper urinary tract and bladder capacity [6].
In particular, considerations were given on how to evaluate a neurogenic bladder in uncooperative children. Intravesical pressure might not be reliably predicted owing to the inability to maintain constant abdominal pressure during UDS because of the uncomfortable posture necessary, especially in these children. Therefore, we considered that CMG and CIC with faithful voiding diaries were more preferable than traditional UDS. Serial CMGs might be a good strategy to determine the timing of indwelling catheter removal in case 1, assuming that the detrusor pressure at the endpoint of storage reflects that of the starting point of bladder emptying. Furthermore, CIC with voiding diaries is considered to serve as a good method to follow up the recovery pattern of voiding in case 2.
In conclusion, the individualized approach is important considering several points including the underlying pathology and limitations of the uncoordinated patient. Furthermore, we suggest that efforts should be made to determine when to recover normal urination patterns and how to assess bladder function during recovery. In addition, clinicians should determine which tool would be helpful in assessing detrusor function at a particular point, especially in severely mentally and physically disabled pediatric patients.
Further studies on large samples are expected to determine the relationships among the types of neurogenic bladder after seizures, locations of the partial seizures, and types of seizures.
ACKNOWLEDGMENTS
This work was supported by a clinical research grant from Pusan National University Hospital in 2018.
AUTHOR CONTRIBUTION
Conceptualization: Shin YB. Writing – original draft: Park HE, Shin YB. Writing – review & editing: Park HE, Lee JS, Kim DM, Shin YB. Approval of final manuscript: all authors.
Fig. 1.
X-ray of the abdomen showed a mass, which was later revealed to be the distended bladder of the patient in case 2.
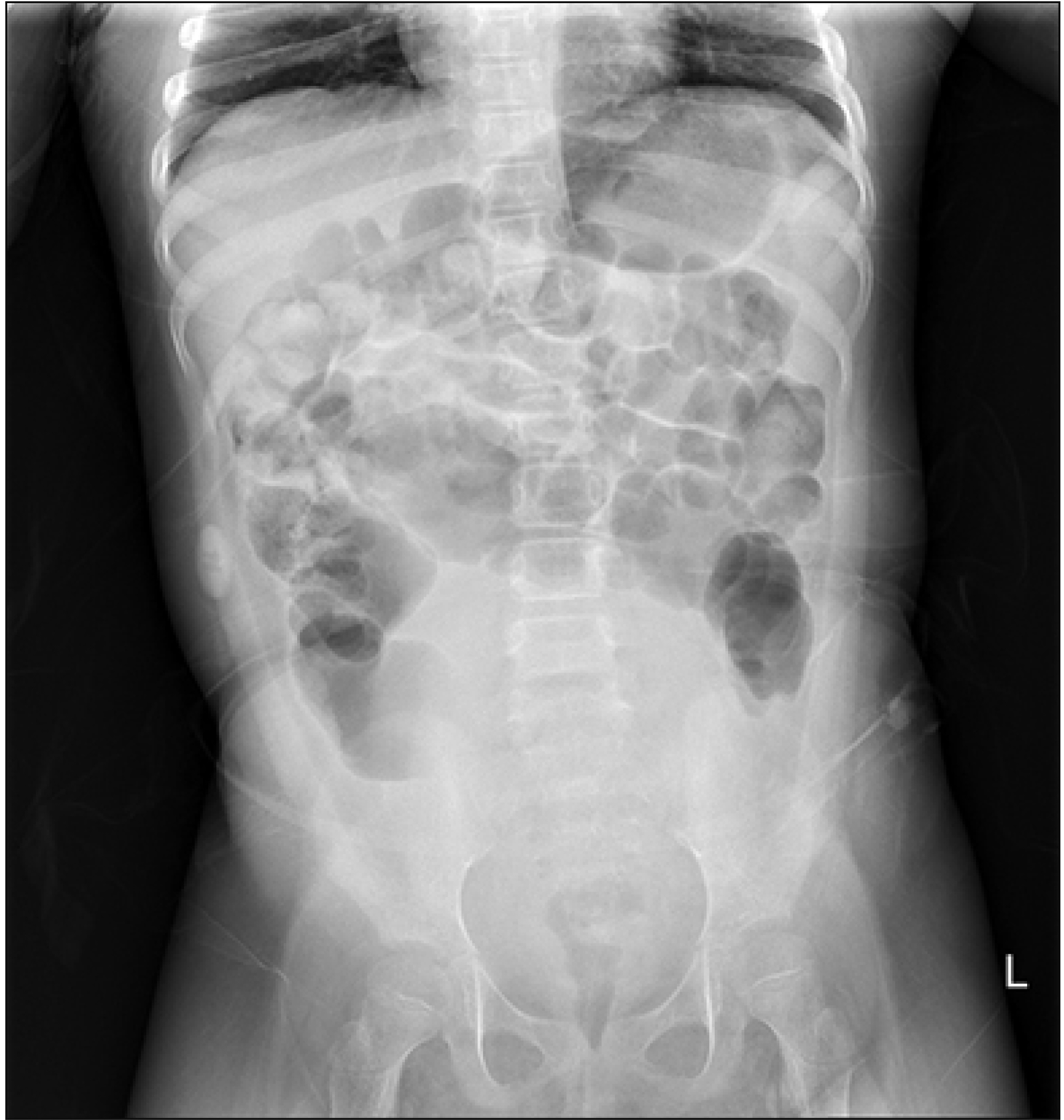
Table 1.
Serial cystometrogram findings of case 1
Serial tests were performed to predict when detrusor activity is observed to self-void. Until the 3rd test, the intravesicular pressure showed a gradual increase pattern, with maximal pressure up to 13 cmH2O. At the 4th follow-up study, the surge of intravesicular pressure was notable, reflecting that the timing for trying the initiation of self-voiding might be appropriate.
REFERENCES
2. Nevo A, Mano R, Livne PM, Sivan B, Ben-Meir D. Urinary retention in children. Urology 2014;84:1475-9.


3. Fowler CJ, Griffiths D, de Groat WC. The neural control of micturition. Nat Rev Neurosci 2008;9:453-66.




4. Selius BA, Subedi R. Urinary retention in adults: diagnosis and initial management. Am Fam Physician 2008;77:643-50.

- TOOLS







