INTRODUCTION
Carpal tunnel syndrome (CTS) is a common medical condition, in which the median nerve is compressed at the wrist, leading to paresthesia, numbness, and muscle weakness of the hand [
1]. Diabetic sensorimotor polyneuropathy (DSP) is known to be a length-dependent, symmetrical polyneuropathy that mainly affects the large nerve fibers within the body [
2,
3]. The prevalence of CTS was reported to be 2% in the general population, 14% in diabetic patients without DSP, and 30% in diabetic patients with DSP [
4]. CTS is traditionally diagnosed based on a combination of history of symptoms, physical examination, and electrodiagnostic study [
1]. However, ultrasonography (US) has also played an adjuvant role in the diagnosis of CTS by evaluating the enlargement of the cross-sectional area (CSA) of the median nerve and the abnormality of the adjacent soft tissue [
5,
6]. Several studies have attempted to determine the absolute cutoff values of median nerve CSA for diagnosing CTS, but no consensus regarding the absolute diagnostic value has been established yet [
5,
7-
9]. However, since absolute CSA can be affected by anthropometric character, sex, and presence of polyneuropathy, the relative CSA value is theoretically more accurate in the diagnosis of CTS. According to a report, the peripheral nerves of patients with DSP show diffuse enlargement at the whole nerve length, which represents sonographically larger CSA of the peripheral nerves [
10]. Moreover, in a study of median nerve US in diabetic patients, the median nerve CSA in the carpal tunnel of DSP patients was greater than that in healthy individuals or in patients without DSP [
11]. In patients with CTS combined with DSP, the focal enlargement process may also be added to the already enlarged median nerve. Thus, measuring only the absolute CSA of the median nerve may render false-positive results when diagnosing CTS combined with DSP.
Therefore, the objective of this study was to investigate the optimal US evaluation method for diagnosing CTS in patients with DSP.
RESULTS
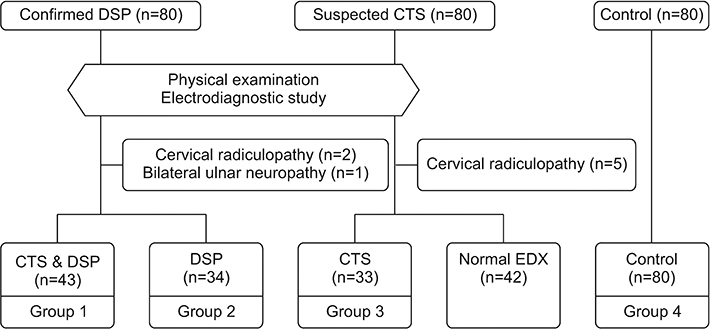
The participants’ characteristics are summarized in
Table 1. There were no significant differences in terms of age, sex, weight, height, and BMI among the four groups. There were no significant differences in the CTS grade between groups 1 and 3, and in diabetes duration and HbA1c between groups 1 and 2.
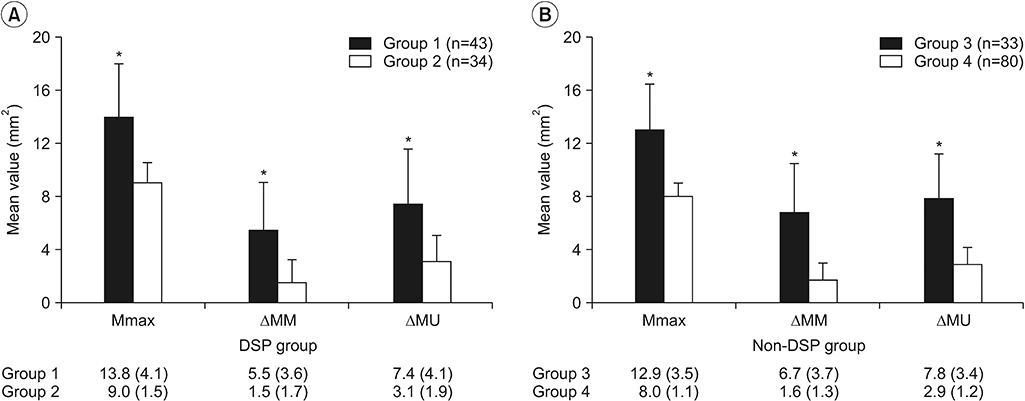
To investigate the influence of CTS and DSP on the CSA of the peripheral nerves, we compared the mean sonographic parameters between the CTS and non-CTS patients in each of the DSP and non-DSP groups (
Fig. 3).
In the DSP group, group 1 (n=43) showed larger primary US parameters than group 2 (n=34) (
Fig. 3A): Mmax (13.8 vs. 9.0 mm
2; 95% confidence interval [CI], 3.4–6.1; p<0.001), ΔMM (5.5 vs. 1.5 mm
2; 95% CI, 2.8–5.2; p<0.001), and ΔMU (7.4 vs. 3.1 mm
2; 95% CI, 2.9–5.7; p<0.001). However, the reference parameters (Mf and Upi) were not different between groups 1 and 2: Mf (8.0 vs. 7.5 mm
2; 95% CI, 0.4–0.3; p=0.204), and Upi (6.4 vs. 5.9 mm
2; 95% CI, -0.1–1.0; p=0.120).
In the non-DSP group, similar patterns were observed compared with the DSP group. Group 3 (n=33) showed larger US variables than group 4 (n=80) (
Fig. 3B): Mmax (12.9 vs. 8.0 mm
2; 95% CI, 3.6 to 6.2; p<0.001), ΔMM (6.7 vs. 1.6 mm
2; 95% CI, 3.7 to 6.4; p<0.001), ΔMU (7.8 vs. 2.9 mm
2; 95% CI, 3.6 to 6.1; p<0.001). However, the reference parameters (Mf and Upi) were not different between groups 3 and 4: Mf (6.2 vs. 6.3 mm
2; 95% CI, -0.6–0.4; p=0.705), and Upi (5.1 vs. 5.0 mm
2; 95% CI, -0.3–0.5; p=0.645).
To investigate the influence of DSP on peripheral nerves, we compared the mean sonographic parameters between the DSP and non-DSP patients in each of the CTS and the non-CTS groups. Group 1 (n=43) showed significantly larger reference parameters (Mf and Upi) compared with group 3 (n=33): Mf (8.0 vs. 6.2 mm2; 95% CI, 1.3–2.7; p=0.000), and Upi (6.4 vs. 5.1 mm2; 95% CI, 0.7–1.8; p=0.000). However, Mmax, ΔMM, and ΔMU did not show significant differences between groups 1 and 3: Mmax (13.8 vs. 12.9 mm2; 95% CI, -0.9–2.7; p=0.330), ΔMM (5.5 vs. 6.7 mm2; 95% CI, -2.8–0.5; p=0.181), and ΔMU (7.4 vs. 7.8 mm2; 95% CI, 3.6–6.1; p=0.685).
In the non-CTS group, group 2 (n=34) showed significantly larger US parameters than group 4 (n=80): Mmax (9.0 vs. 8.0 mm2; 95% CI, 0.5–1.5; p=0.000), Mf (7.5 vs. 6.3 mm2; 95% CI, 0.6–1.7; p=0.000), and Upi (6.4 vs. 5.1 mm2; 95% CI, 0.5–1.3; p=0.000). However, ΔMM and ΔMU did not show significant differences between groups 2 and 4: ΔMM (1.5 vs. 1.6 mm2; 95% CI, -0.7–0.5; p=0.671) and ΔMU (3.1 vs. 2.9 mm2; 95% CI, -0.5–0.7; p=0.652).
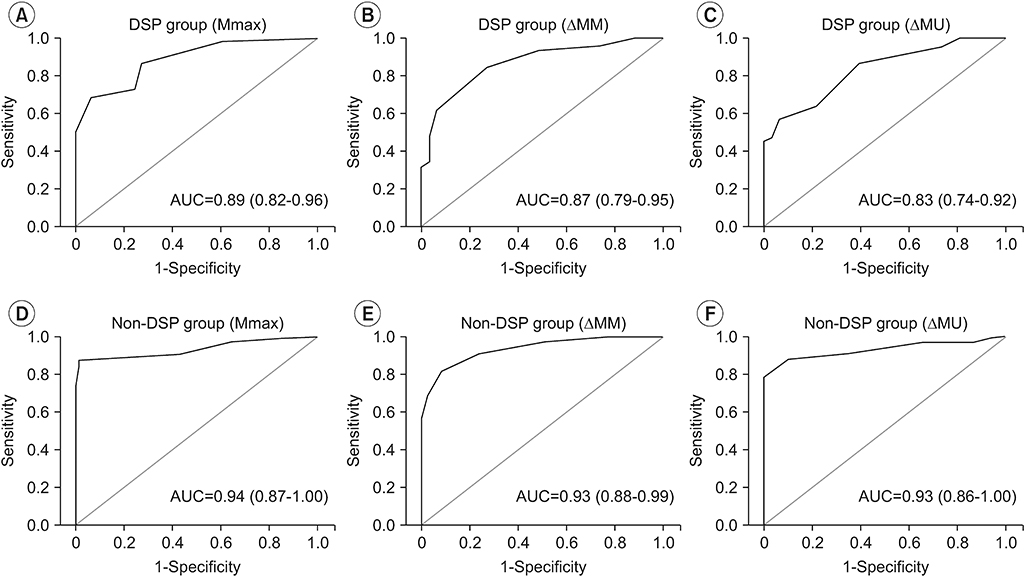
The ROC curve analysis was performed to identify the sensitivity and specificity of the US parameters in diagnosing CTS in the DSP and non-DSP groups (
Fig. 4,
Table 2). Based on the ROC curves analyses, the following Mmax, ΔMM and ΔMU cutoff values were chosen to diagnose CTS: Mmax thresholds that showed the greatest sensitivity and specificity were 9.5 and 11.5 mm
2 in the non-DSP and DSP groups, respectively; ΔMM and ΔMU thresholds of 2.5 and 4.5 mm
2, respectively, had the greatest sensitivity and specificity in both the DSP and non-DSP groups. The diagnostic accuracy of each US evaluation method (Mmax, ΔMM, and ΔMU) was analyzed using pairwise comparison tests. In the DSP group, the areas under the ROC curves were 0.89 (95% CI, 0.82–0.96) for Mmax, 0.87 (95% CI, 0.79–0.95) for ΔMM, and 0.83 (95% CI, 0.74–0.92) for ΔMU. In the non-DSP group, the areas under the ROC curves were 0.94 (95% CI, 0.87–1.00) for Mmax, 0.93 (95% CI, 0.88–0.99) for ΔMM, and 0.93 (95% CI, 0.86–1.00) for ΔMU. There was no statistically significant difference between the three methods in the DSP and non-DSP groups.
DISCUSSION
In our study, we determined that Mmax, ΔMM, and ΔMU could be useful for diagnosing CTS in patients with DSP.
The mechanism of nerve swelling in diabetic neuropathy has been studied. The wet weights and water content of the sciatic nerves of diabetic rats were increased compared with those of normal rats [
17]. It has been hypothesized that this increased water content is related to increased aldose reductase conversion of glucose to sorbitol [
18]. In the peripheral nerve, aldose reductase has been localized to the Schwann cell [
19]. The slow penetration of sorbitol of cell membranes [
20] can result in osmotic swelling. Given this nerve enlargement in patients with diabetic neuropathy, US has been increasingly used for diagnosing diabetic neuropathy. In a previous study, the CSA of the median nerve of diabetic patients with DSP was significantly larger than that of normal healthy subjects [
11]. In the present study, the Mmax of the median nerve had a tendency to be larger in the DSP group than in the non-DSP group.
Some studies have attempted to ascertain the usefulness of US for diagnosing CTS in patients with DSP. US can be performed non-invasively and easily compared with electrodiagnostic studies. In addition, treatment such as injection therapy can be conducted simultaneously with diagnosis, and adjacent structures can be evaluated if needed. A previous cross-sectional casecontrol study reported that the CSA of the median nerve of patients with CTS was similar to that of patients with CTS and DSP [
21]. Another research study showed a similar result at the wrist level, but reported a significant difference in the CSA of the median nerve in the forearm level between patients with CTS only and those with CTS and DSP [
16]. This result was considered to be due to the diffuse nerve enlargement from the wrist to the forearm in patients with DSP. Similar to previous studies, there were no significant differences in the US values between patients with CTS and DSP (group 1) and patients with CTS only (group 3) in the present study.
Some US parameters have been suggested for the diagnosis of CTS in patients with DSP. Some studies have reported that the wrist-to-forearm ratio (WFR) of the nerve diameter or CSA determined by US could be useful for diagnosing the comorbidity of CTS with DSP [
16,
22]. However, one of the studies reported that the WFR has a low diagnostic accuracy and should be used with caution [
22]. In addition, the study evaluating US for the diagnosis of CTS in patients with DSP reported that US parameters, including CSA, WFR, and wrist-forearm difference, were not significantly different between patients with CTS plus DSP and patients with DSP only [
23]. Hence, the aforementioned ultrasound parameters cannot totally replace electrodiagnostic studies in diagnosis of CTS.
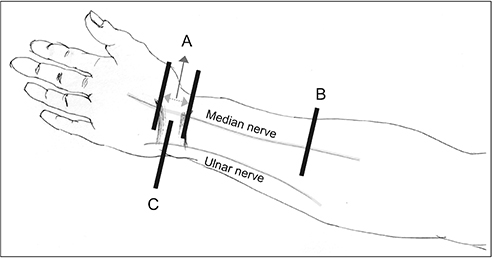
In this study, a significant difference was found in Mmax, ΔMM, and ΔMU between patients with CTS and DSP (group 1) and patients with DSP only (group 2), which is contrary to the results of a previous study using the wrist-forearm difference. This discrepant outcome was considered to be due to the use of the maximal value in measuring the dilated median CSA in the present study. If measured at the fixed site, the CSA of the median nerve might not reflect the true neurophysiologic status of the nerve. Additionally, the CSA of the ulnar nerve could be a good standard parameter for diagnosing CTS in patients with DSP, because CTS mainly concerns pathogenesis of the median nerve, due to its location in the carpal tunnel.
In a study reporting the usefulness of US in diagnosing CTS in patients with DSP [
16], the cutoff value of the median nerve CSA at the wrist level was 11.6 mm
2. Similarly, the cutoff value of Mmax was 11.5 mm
2 in this study. However, the sensitivity and specificity were higher in this study. Moreover, we determined that the cutoff value was 9.5 mm
2 in the non-DSP group. Therefore, to diagnose CTS, the median nerve CSA should be measured as a maximal value through the carpal tunnel from the hamate bone level to the radioulnar joint level, and should be used as a different value in DSP and non-DSP groups.
The cutoff values of ΔMM and ΔMU for diagnosing CTS were 2.5 and 4.5 mm2, respectively. In the ROC curve analysis, the Mmax, ΔMM, and ΔMU were not significantly different between the DSP and non-DSP groups. Furthermore, ΔMM and ΔMU can be obtained through simple subtraction.
There were some limitations to this study. First, we evaluated the Mmax among the CSAs values of median nerve at three levels: the hamate bone level, the pisiform bone level, and the radioulnar joint level. Thus, the maximal value among these three might not be the maximal value of the median nerve. Second, the US study was only conducted once by a single physiatrist. Thus, no interrater and intra-rater reliability tests could be performed. Future studies should be performed by multiple physiatrists with reliability tests. Third, we used a neurophysiologic classification to assess the electrophysiologic severity of CTS without considering DSP. However, pathologic alteration of peripheral nerves in patients with DSP might affect the results of CTS severity and lead to bias. Finally, we recruited patients with DSP whose diagnosis was confirmed by NCS within a year, without additional electrodiagnostic assessment for DSP after recruitment for this study. Thus, the neurophysiologic status of the nerves could differ between the times of diagnosis and recruitment. Therefore, we could not analyze the correlation between electrophysiologic parameters and US features.
In conclusion, US could be considered as an alternative method for diagnosing CTS in patients with DSP. The US parameters of Mmax, ΔMM, and ΔMU are expected to be used with ease in clinical practice.