Knee Extensor Strength Measurement in Patients With Limited Physical Activity Using a Supine Dynamometer Anchoring Frame
Article information
Abstract
Objective
To investigate the reliability of knee extensor strength measurements using a supine hand-held dynamometer (HHD) anchoring frame in patients with limited physical activity. Although an HHD is suitable for bedside use, its inter-rater reliability is low because measurements can be influenced by tester strength.
Methods
Maximal knee extensor isometric strength was measured using an HHD anchored to the supine frame. Three trials of three maximal contractions were assessed by two raters.
Results
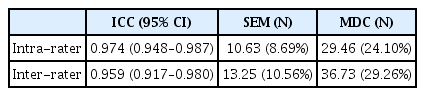
A total of 33 inpatients who were non-ambulatory due to acute illness participated in the study. The intraclass correlation coefficients were 0.974 (inter-rater) and 0.959 (intra-rater). The minimal detectable changes in intra- and inter-observer measurements were 29.46 N (24.10%) and 36.73 N (29.26%), respectively. The limits of agreement ranged from -19.79% to 24.81% for intra-rater agreement and from -21.45% to 37.07% for inter-rater agreement.
Conclusion
The portable dynamometer anchoring system can measure the isometric strength of the knee extensor reliably in the supine position, and could be used for measurements in patients who have difficulty visiting the laboratory and maintaining a seated posture.
INTRODUCTION
Muscle weakness is an independent risk factor for morbidity and mortality [1,2], and is an important contributor to long-term physical impairments [3]. It is well known that long-term hospitalization due to medical or surgical conditions can result in detrimental physiological effects on muscle strength and physical activity; this functional decline can lead to further inactivity, thus entering a vicious cycle [4].
Assessment of muscle strength is important for evaluating the outcomes of clinical interventions in order to break this vicious cycle. The manual muscle test (MMT), which uses the Medical Research Council (MRC) grading system, is the most common method of muscle strength measurement in busy clinical settings. However, the MMT is prone to error and only poorly able to distinguish subtle differences, as it relies on an examiner’s judgment [5]. In particular, the inter-rater reliability of the MMT is not sufficient for distinguishing between grades 4 and 5 muscle strength [6].
The isokinetic dynamometer (IKD) is considered the gold standard for muscle strength testing. However, it is a large tool with limited portability [7]; thus, patients are required to visit the laboratory to undergo measurements. As a result, it is impractical for use in patients who cannot ambulate independently or in those who have several monitoring devices or drains.
The hand-held dynamometer (HHD) is a portable device that provides a quantified measurement of strength. Compared with an IKD, its convenience, small size, and low cost make it more suitable for bedside use [7]. However, the inter-rater reliability is low because the measurements can vary depending on tester strength [8]. To increase reliability, recent studies have attempted to affix an HHD to a frame rather than having it held by the examiner [9-12].
Recently, Sung et al. [13] suggested the use of a portable dynamometer anchoring system that can measure knee extensor strength in the supine position, and confirmed its reliability and validity in 39 healthy people. This system can be appropriately applied to cases where it is difficult to move the patients to the laboratory or for patients who have difficulty maintaining a sitting position during the test, since the system can measure strength in the supine position. The aim of the present study was to investigate the reliability of knee extensor strength measurement using a supine HHD anchoring frame for patients with limited physical activity.
MATERIALS AND METHODS
Subjects
Patients who were non-ambulatory due to long-term immobilization or neurologic conditions, and older than 18 years of age were enrolled. Patients were excluded if they had a history of traumatic spinal or lower extremity injury within the past 6 months, an inserted femoral catheter, or were unable to give consent and understand the procedures of the experiment. The Institutional Review Board of Seoul National University Hospital approved the study and signed (No. 1804-077-936), written informed consent forms were obtained. The participants were informed of the study purpose and procedures prior to enrollment.
Portable dynamometer anchoring system
The portable dynamometer anchoring system consisted of an HHD attached to a custom-designed portable mechanical frame (Fig. 1). The frame bar perpendicular to the tibia was designed to move up and down, according to leg thickness. The other two frame bars, which were designed to move back and forth depending on leg length, were fixed by hand knob tightening screws. The frame was designed at an angle of 145° to flex the knee at 35°. The angle of 35° was chosen keeping in mind previous study results, which reported that high-level surface electromyography activity was observed when the knee joint was flexed at 35° [14]. Studies measuring knee extensor strength with the knee joint flexed at 35° in the HHD test showed good reliability [9,13,15]. Four U-shaped rings were placed on the corners of the frame to connect the belts for fixing the device to the bed. The thighs of the participants can be fixed using a Velcro strap to minimize hip flexion movement [13].
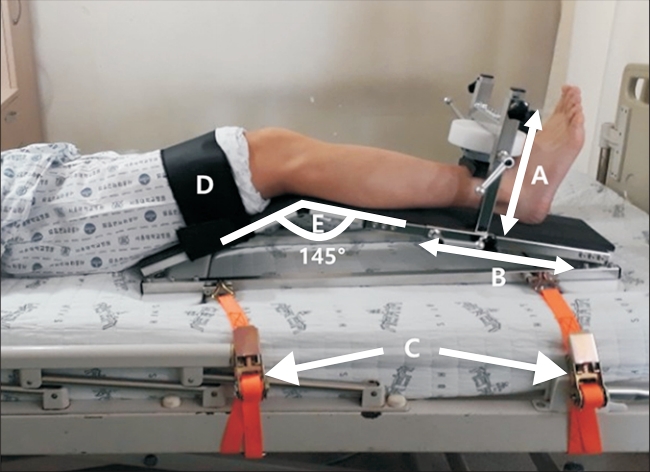
Portable dynamometer anchoring system in a supine position. A, the frame can be moved to adjust the hand-held dynamometer (HHD) depending on leg thickness; B, the frame can be moved to adjust the HHD depending on leg length; C, belts that fix the frame to the bed; D, Velcro strap to fix the patient’s thigh to minimize hip flexion movement; and E, the frame was designed at an angle of 145° to flex the knee to 35°.
Isometric knee extension strength was assessed with a microFET IITM (Hoggan Health Industries, Draper, UT, USA), which is a battery-operated load cell system with a digital reading of peak force ranging from 12.1 N to 1,334.5 N, in 0.4 N increments. The HHD was placed 5 cm above the upper margin of the lateral malleolus [13].
Measurement procedure
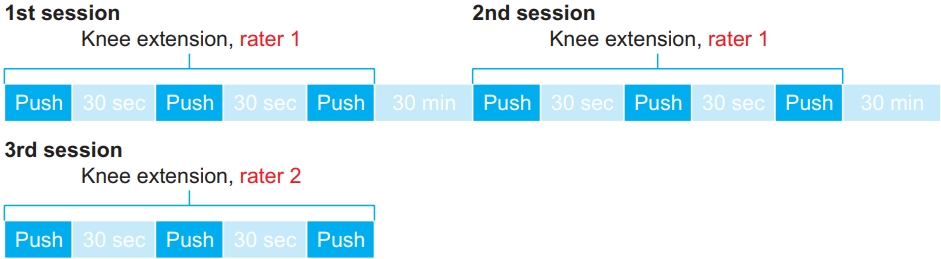
During the measurement, the subject was in the supine position with their arms lightly positioned on their chest. The examiner adjusted the position of the HHD depending on leg length and thickness. Before the measurement, the subjects performed knee extension of the dominant leg several times to become familiar with the device. The measurements consisted of three total sessions consisting of three 5-second maximal isometric contractions of the dominant knee extensors, in each trial [13].
The measurements were evaluated by two physiotherapists acting as examiners. The first and second sessions were evaluated by one rater, while the third was evaluated by the other rater. The order of the raters was randomized. The interval between sessions was 30 minutes, and the interval between test repetitions was 30 seconds (Fig. 2).
The measurement began with a recorded sound (“kick”). When a subject extended their knee, the examiner pressed down on both the anterior superior iliac spine regions of the pelvis to prevent pelvic rotation. Participants were instructed to inform the examiner of any pain or discomfort during the test, and the test was allowed to be stopped at any time, on request [13]. Participants were not provided encouragement during the test or given knowledge of their results between trials.
After the measurements were taken, one investigator assessed the MRC sum score and the de Morton Mobility Index to evaluate the functional status of the subject.
Statistical analyses
The normality of the data was checked using the Kolmogorov-Smirnov test. To evaluate relative reliability, a two-way random effect model of the intraclass correlation coefficient (ICC) was used for the estimation of intra- and inter-rater reliabilities [16]. The ICCs were interpreted according to the following guidelines: based on the 95% confidence interval of the ICC, values less than 0.5, between 0.5 and 0.75, between 0.75 and 0.9, and greater than 0.9 were indicative of poor, moderate, good, and excellent reliability, respectively [17].
To ensure absolute reliability, several parameters were calculated according to the COnsensus-based Standards for the selection of health Measurement INstruments (COSMIN) quality assessment [18]. The standard error of mean (SEM) was calculated using the following formula:
The 95% limits of agreement (LoA) were calculated as the difference against the mean plot,
A repeated-measures ANOVA was conducted to test for learning and fatigue effects with the three maximal isometric knee extension strength measurements of each session [23]. All statistical analyses were performed using SPSS version 23 for Windows (IBM, Armonk, NY, USA).
RESULTS
A total of 40 patients were initially included in the study. Of them, 6 refused to undergo the test due to fatigue, and one patient dropped out due to knee pain during the test. A total of 33 patients were analyzed, among them 18 men and 15 women (median age, 75.0 years; interquartile range, 60.5–89.5). The demographics and characteristics of the patients are presented in Table 1. All subjects were non-ambulatory, 15 of whom were unable to sit unsupported in a chair.
Table 2 shows the maximal isometric knee extension strength values. The relative reliability of the anchoring system using an HHD, including the ICCs and 95% CIs, was excellent for the intra- and inter-observer measurements. The MDCs of the intra- and inter-observer measurements were 29.46 N (24.10%) and 36.73 N (29.26%), respectively (Table 3).
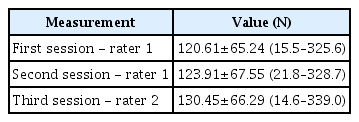
Maximal isometric knee extension strength values using a portable dynamometer anchoring system (n=33)
The average difference between the two sessions performed by the first rater for intra-observer measurements was 3.31 N (2.51%), and the LoA ranged from -26.15 to 32.77 N (-19.79% to 24.81%). The average difference between the first and second raters for inter-observer measurements was 9.84 N (7.81%), and the LoA ranged from -26.89 to 46.57 N (-21.45% to 37.07%). The distributions are represented in the Bland-Altman plot (Fig. 3).
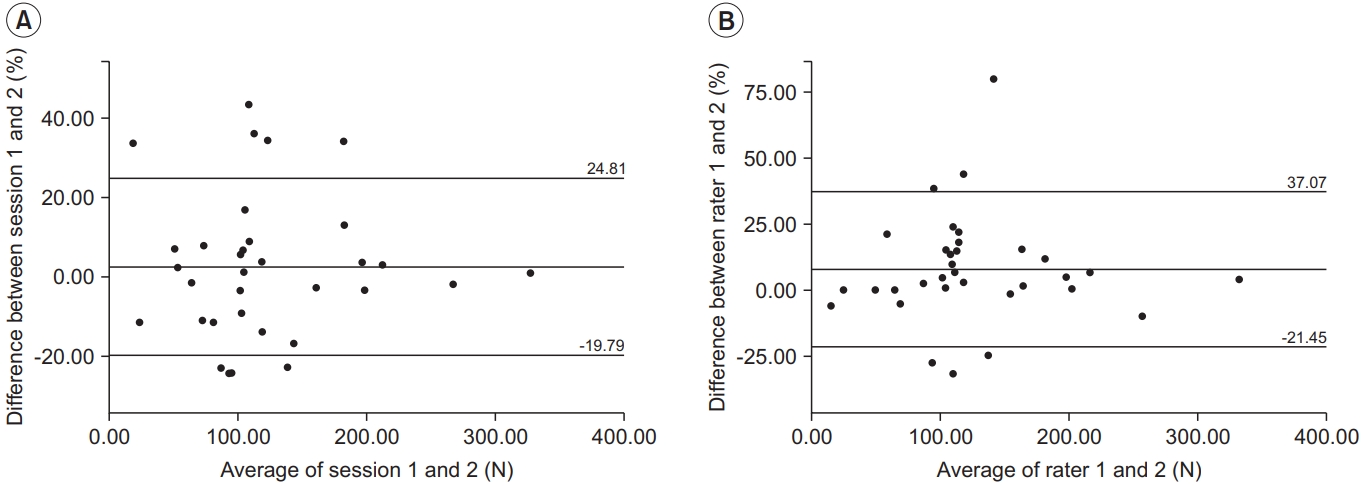
Distribution from Bland-Altman plots for the mean difference and limits-of-agreement of (A) intra-rater measurements and (B) inter-rater measurements.
The ANOVA test for repeated measures yielded no significant changes (p=0.924) among the three sessions, indicating that there were no learning effects from the first to the third measurements in a session.
DISCUSSION
The present study evaluated the reliability of the portable dynamometer anchoring system in patients with limited physical activity. This system showed excellent intraand inter-rater reliabilities for maximal isometric knee extensor strength measurements, and the relative reliability calculated by ICC was excellent (intra-rater=0.974, inter-rater=0.959). These results are similar to those of previous HHD studies. Lu et al. [10] reported excellent ICCs for the intra- and inter-rater reliabilities of knee extensor strength measurements (intra-rater=0.91–0.94, inter-rater=0.98) using a fixation structure in the sitting position. In the study by Jackson et al. [24] that used a portable stabilization device in the sitting position, the ICC for intra-rater reliability of knee extensor strength measurements was 0.93. However, these studies measured the knee extensor strength in healthy adults in the sitting position, which is difficult to replicate in severely deconditioned patients who are unable to balance and kick in that position.
A few studies that used fixation devices have reported the reliability of HHD for measuring knee extensor strength in a clinical population. In the study by Koblbauer et al. [11], patients awaiting total knee arthroplasty were assessed in the sitting position; in this study, the HHD was modified with straps to support the device. The MDCs for intra- and inter-rater reliabilities were 19.0%–31.4% and 21.7%, respectively. In a study by Gagnon et al. [12], the MDC for inter-rater reliability was 23.84%–36.50% in patients who had undergone hip or knee arthroplasty; in this study, a chair-fixed dynamometer system was developed and used. The HHD was mounted on a rigid support, which was able to move along a shaft fixed to a chair.
Several studies have reported the reliability of an IKD for measuring knee extensor strength in a clinical population. In the study by Kean et al. [25], the MDC for interrater reliability using an IKD in patients with knee osteoarthritis was 17.73%. Another IKD study in post-stroke patients reported an intra-rater MDC of 25.34% [26]. In their study of chronic obstructive pulmonary disorder (COPD) patients, Machado et al. [27] found the MDC to be 22.05% in IKD measurements.
Few studies have examined knee extensor strength using an HHD in intensive care unit (ICU) patients, who should undergo measurements while in bed. Baldwin et al. [28] reported an MDC of 47.3% for intra-rater reliability using an HHD in ICU patients without the use of a fixation device. Rousseau et al. [29] designed a highly standardized dynamometer for measuring knee extensor strength in ICU patients in the supine position. The MDC in that study was 17.13%–27.33%. Although the MDC was comparable, the highly standardized dynamometry developed therein seems difficult to install, making it less convenient to use.
The MDC is a decision limit from a change in variability or measurement error. In this study, the MDCs were 29.46 N (24.10%) for intra-rater reliability and 36.73 N (29.26%) for inter-rater reliability. The MDC percentage values reported in the current study were lower than those reported in previous studies using the HHD anchoring frame, and comparable to those using an IKD. We infer that the reasons for this are as follows. First, the supine position may have affected the results. The supine measurement technique was found to be stable for the subjects because it was easier for them to maintain the testing position, compared with the sitting posture [15]. Second, when the patients were kicking the dynamometer, the examiner pressed both sides of the anterior superior iliac spine to prevent compensatory rotation of the pelvis. This stabilization technique cannot be performed in a sitting position. Third, the frame was fixed to the patient’s bed using a non-elastic belt (Fig. 1). The belts were inserted into the four U-shaped rings on the frame and pulled towards the bed to fix the frame, thus minimizing shaking during kicking.
The system developed in this study can only measure knee extensor strength. In deconditioned patients, lower limb weakness is more severe than trunk weakness [30]. Specifically, since muscle atrophy is pronounced in knee extensor muscles, the knee extensor strength has been evaluated as an indicator of deconditioning in patients on bed rest [31]. In addition, knee extensors are essential for walking and reflect functional states well [32]. Therefore, knee extensor strength assessment can be considered as a parameter for surveilling muscle weakness and functional outcomes in severely deconditioned patients due to acute illness.
Seymour et al. [33] reported that the quadriceps cross-sectional area estimated by ultrasonography was related to strength in COPD patients, while Grimm et al. [34] suggested that muscle ultrasound could be useful for screening critical illness neuromyopathy. However, it has been reported that estimating muscle volume is not useful for predicting functional outcomes [34]. Direct muscle strength measurement, as in this study, might be more likely to predict a functional outcome than the evaluation of muscle function indirectly through imaging studies. For example, the knee extensor strength measurement method presented in this study could be used for rehabilitation of patients in the ICU. This system can be simply installed on a bed using only four ropes, in about 10 minutes, and the test can be completed in less than 5 minutes. This HHD anchoring system is suitable for bedside measurement of knee extensor strength. In future studies, it may be possible to investigate how muscle strength directly measured in deconditioned patients is associated with functional recovery after treatment for acute illness.
The current study has several limitations. First, although the participants of this study had similar limitations in physical function, such as walking and maintaining sitting posture, they were from diverse disease groups. The reliability of measuring muscle strength using the supine HHD anchoring frame may differ with different disease groups. Second, the participants in this study used air mattresses to prevent pressure ulcer formation related to their limited mobility. In this study, the frame was placed on the mattress and the muscle strength was measured; thus, the measurement could have been affected. However, it would be difficult to remove the air mattresses to measure leg strength in actual clinical situations. Finally, bias from the two examiners could not be completely eliminated because the examiners were not blinded to the test results. However, since the examiner could not control the dynamometer, which was attached to the portable dynamometer anchoring system, and could only press down on the anterior superior iliac spine regions of the pelvis to prevent pelvic rotation during the measurements, we believe that there was little chance of bias.
In conclusion, the portable dynamometer anchoring system designed in this study can measure the isometric strength of the knee extensor reliably in the supine position; therefore, it can measure the strength in patients with limited physical activity who have difficulties in moving to the laboratory and in maintaining a sitting posture for the measurement.
Notes
No potential conflict of interest relevant to this article was reported.
Acknowledgements
This work was funded by the Korea Workers’ Compensation and Welfare Service.
Notes
Conceptualization: Shin HI. Methodology: Lee MY, Sung KS, Ham H, Yi YG, Shin HI. Formal analysis: Lee MY, Yi YG. Funding acquisition: Shin HI. Project administration: Lee MY, Yi YG. Visualization: Lee MY, Sung KS. Writing – original draft: Lee MY, Sung KS, Yi YG. Writing – review and editing: Lee MY, Shin HI. Approval of final manuscript: all authors.